Beautiful Plants For Your Interior
Summary
3-Methylbutyrfentanyl (3-MBF) is an opioid analgesic, considered an analog of butyrfentanyl.
Like fentanyl, the side effects of fentanyl analogs, including 3-MBF, encompass symptoms such as itching and nausea. Of particular concern is the potential for severe respiratory depression, which can be life-threatening. Notably, fentanyl analogs have been associated with numerous fatalities across Europe and the former Soviet republics. This pattern of harm became pronounced with a resurgence in use, particularly in Estonia during the early 2000s, and novel derivatives of these substances continue to emerge.
| Identifiers | |
|---|---|
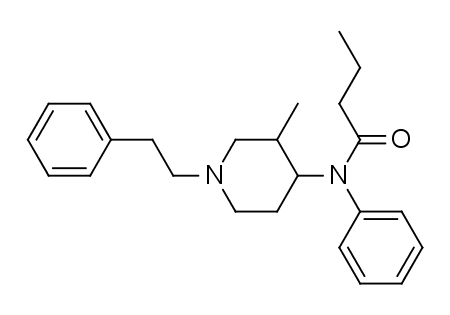
| IUPAC name | |
| CAS Number | 97605-09-9 |
|---|---|
| PubChem CID | 86130531 |
| ChemSpider | 57434313 |
| UNII | 875L53T89N |
| Chemical and physical data | |
| Formula | C24H32N2O |
| Molar mass | 364.533 g·mol−1 |
FAQ
- What is 3-Methylbutyrfentanyl (3-MBF)?
- 3-Methylbutyrfentanyl, often abbreviated as 3-MBF, is an opioid analgesic. It is classified as an analog of butyrfentanyl.
- What are the potential side effects of 3-MBF?
- Like other fentanyl analogs, the side effects of 3-MBF may include itching, nausea, and, most critically, the risk of severe respiratory depression, which can be life-threatening.
- How does 3-MBF compare to fentanyl?
- 3-MBF is structurally related to buying fentanyl and falls within the family of fentanyl analogs. These analogs share similarities with fentanyl in terms of their effects and risks.
- Has 3-MBF been associated with harm or fatalities?
- Like other fentanyl analogs, 3-MBF has been linked to multiple fatalities, especially in Europe and the former Soviet republics. The resurgence in the use of these substances, starting in Estonia in the early 2000s, has contributed to this pattern of harm.
- Is 3-MBF legal or regulated in any way?
- The legal status of 3-MBF can vary by region. It’s important to stay informed about your specific area’s regulatory status and potential restrictions.
- Is there any legitimate medical use for 3-MBF?
- As of my last knowledge update in September 2021, 3-MBF is not approved for medical use. It is primarily encountered in the context of illicit or non-medical use.
- Where can I find more information about 3-methylbutyrfentanyl?
- For more comprehensive information about 3-methylbutyrfentanyl, consult scientific literature, relevant research studies, and authoritative sources. Additionally, stay updated on any changes in its legal status and evolving safety information.
References
- Drug Enforcement Administration, Department of Justice (February 2018). “Schedules of Controlled Substances: Temporary Placement of Fentanyl-Related Substances in Schedule I. Temporary amendment; temporary scheduling order.” Published in the Federal Register.
- Higashikawa Y, Suzuki S (June 2008). “Studies on 1-(2-phenethyl)-4-(N -propionylanilino)piperidine (fentanyl) and its related compounds. VI. Structure-analgesic activity relationship for fentanyl, methyl-substituted fentanyls and other analogues.” Published in Forensic Toxicology.
- Vardanyan RS, Hruby VJ (March 2014). “Fentanyl-related compounds and derivatives: current status and future prospects for pharmaceutical applications.” Published in Future Medicinal Chemistry.
- Jin WQ, Xu H, Zhu YC, Fang SN, Xia XL, Huang ZM, et al. (May 1981). “Studies on synthesis and relationship between analgesic activity and receptor affinity for 3-methyl fentanyl derivatives.” Published in Scientia Sinica.
- Huang ZM, Zhou J, Chen XJ, Zheng WJ, Zhang HP, Chi ZQ, et al. (September 1984). “[Analgesic activity and toxicity of potent analgesics, ohmefentanyl and mefentanyl].” Published in Zhongguo Yao Li Xue Bao = Acta Pharmacologica Sinica.
- Mounteney J, Giraudon I, Denissov G, Griffiths P (July 2015). “Fentanyls: Are we missing the signs? Highly potent and on the rise in Europe.” Published in The International Journal on Drug Policy.